Research Article
DownloadRole of Prolotherapy in Wound Bed Preparation
Dhinesh S1, Ravi Kumar Chittoria2* and Bharat Prakash Reddy J3
1Junior Resident Department of Surgery JIPMER Pondicherry India.
2Professor and Registrar (Academic) Head of IT Wing and Telemedicine Department of Plastic Surgery and Telemedicine JIPMER Pondicherry India.
3General Surgery Senior Resident Department of Plastic Surgery JIPMER Pondicherry India.
Received Date: 11 July 2024, Accepted Date: 17 July 2024, Published Date: 22 July 2024
*Corresponding author: Ravi Kumar Chittoria, Professor and Registrar (Academic) Head of IT Wing and Telemedicine Department of Plastic Surgery and Telemedicine JIPMER Pondicherry India.
Citation: Dhinesh S, Ravi Kumar Chittoria and Bharat Prakash Reddy J. (2024). “Role of Prolotherapy in Wound Bed Preparation”. International Journal of Medical Research and Medical Case Reports, 1(1); DOI: http;/07.2024/ijmrmcr/005.
Copyright: © 2024 Ravi Kumar Chittoria. This is an open-access article distributed under the terms of the Creative Commons Attribution 4. 0 international License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract:
Burn wounds are the major problem all over the world. Many therapies have been introduced for the management of burn wounds. Management of these wounds is often challenging. But there is no well-established method that accelerates the wound healing rate. Prolotherapy is a method that involves injecting some irritant locally in the wound that is claimed to fasten the healing. This article discusses about the role of prolotherapy in wound bed preparation.
Keywords: prolotherapy; wounds.
Introduction:
Prolotherapy is one of the methods that has been used in difficult wounds. Prolotherapy is a procedure in which an irritant is injected or sprayed into the wound that initiate an inflammatory reaction, thought to promote healing of wound. The most common prolotherapy agent used in clinical practice is dextrose, with concentrations ranging from 12.5% to 25%. Dextrose is considered to be an ideal proliferant because it is water soluble, a normal constituent, and can be injected safely into multiple areas and in large quantity. Hypertonic dextrose solutions act by dehydrating cells at the injection site, leading to local tissue trauma, which in turn attracts granulocytes and macrophages and promotes healing. In this article we share our experience of using prolotherapy in the preparation of wound bed.
Materials and Methods:
In this study, a 42 years old male with 38% thermal burns over anterior and posterior part of chest and abdomen (Figure 1) was enrolled and managed at the Department of Plastic Surgery, JIPMER, Puducherry, India in june 2024 for a duration of 1 month. The study was ethical approved by the institutional review board.
He underwent thorough clinical examination, and essential investigations such as Hemoglobin, Total Count, Differential Count, Bleeding Time, Clotting Time, Erythrocyte Sedimentation Rate, Random and/or Fasting Blood Sugar, Serum Creatinine, Blood Urea, HIV, HBsAg, and Complete Urine Examination were conducted to assess anesthesia fitness and rule out underlying systemic conditions. Additionally, wound swabs were cultured to identify the type of organism and its antibiotic sensitivity.
Prolotherapy is used in our patient for promoting the granulation. (figure 2) After 3 weeks of prolotherapy, total body surface area of burns wound was decreased and neoepitheliation occurred.
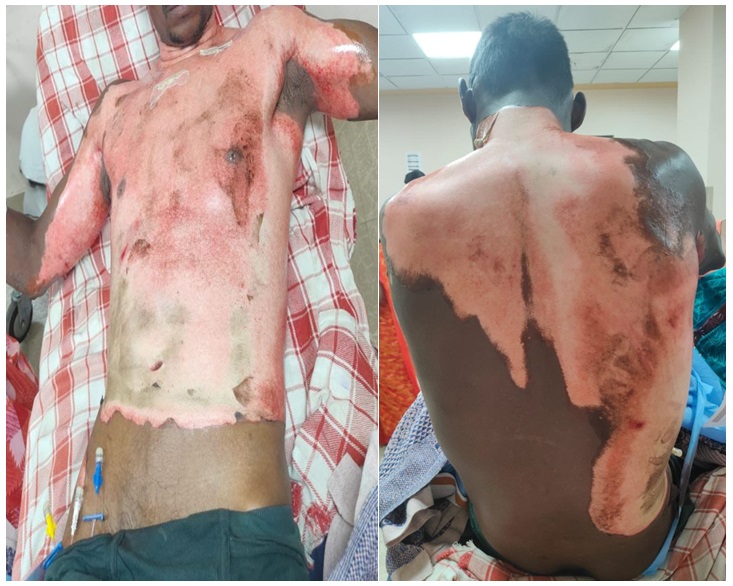
Figure 1: Showing thermal burns over the anterior and posterior part of chest and abdomen at time of presentation (BJWAT Score 32).
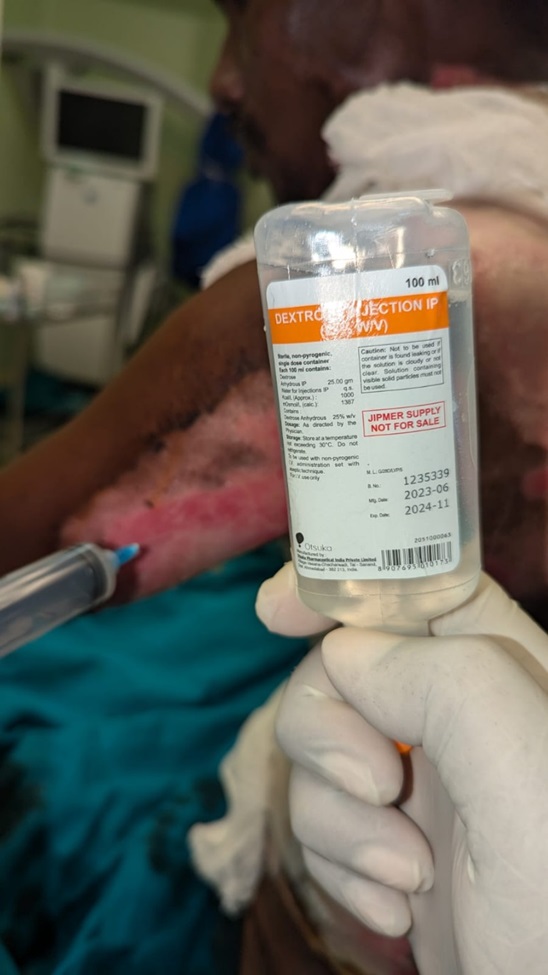
Figure 2: Showing application of prolotherapy over thermal burns.
Results:
After six sessions of prolotherapy over three week’s period, the total body surface area reduced and neoepitheliazation started. No adverse local or systemic effect was noted with the use of Prolotherapy (figure 3).
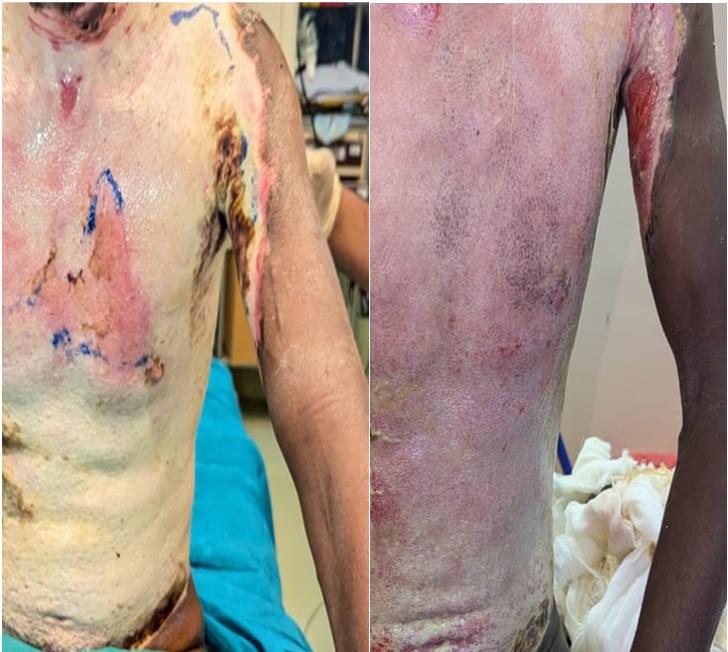
Figure 3: Figure showing condition of the wound before and after prolotherapy over thermal burns (BJWAT wound score - 25)
Discussion:
Multiple agents are used in prolotherapy, some classified as irritants (such as phenol), some as chemoattractants (commonly sodium morrhuate), and others as osmotic agents (commonly dextrose) 1. Although the exact mechanism of prolotherapy is not clear, proponents of the technique believe that the injection of hypertonic dextrose causes cell dehydration and osmotic rupture at the injection site that leads to local tissue injury that subsequently induces granulocyte and macrophage migration to the site, with release of the growth factors and collagen deposition. In vitro studies have shown that even concentrations as low as 5% dextrose have resulted in the production of several growth factors critical for tissue repair. Some of these growth factors include PDGF, TGF-β, EGF, b-FGF, IGF-1, and CTGF [1]. In Vitro studies have shown that the cultivation of cells in high-glucose culture medium can increase PDGF expression. PDGF has multiple pro-reparative effects in skin wounds, including the promotion of angiogenesis, fibroblast proliferation, extracellular production. TGF-β expression is also upregulated by high-glucose. TGF-β is involved in all steps of wound healing including inflammation, angiogenesis, fibroblast proliferation, collagen synthesis, matrix deposition, and remodeling, and wound reepithelialization. Other growth factors upregulated by high glucose include EGF, b-FGF, IGF, and CTGF, all having multiple preparative functions and improves healing in some animal wound models of impaired healing [2, 3]. Some studies on prolotherapy suggest that there are direct effects on collagen synthesis. There is up-regulation of matrix in response to dextrose prolotherapy4. Collagen expression is increased after exposure of patellar tendon fibroblasts to the prolotherapy agents dextrose and thus may contribute to tissue regeneration within a cutaneous wound. Collagen type-I synthesis is also increased in high-glucose cultivation of renal fibroblasts, in a TGF-β-mediated pathway. Changes in the cartilage matrix protein aggrecan are reported in chondrocytes cultured in high-glucose [4, 5], and in patients who have received intraarticular injections of 12.5% dextrose. In our case we have used dextrose 25% as prolotherapy agent. We have used it as adjunct to other modalities. We have not noticed any adverse effect.
Conclusion:
In this study, we found that prolotherapy has a role in the healing of the burn raw area and can be used as an adjuvant therapy for reducing total body surface area and neoeitheliazation. But since it is a single case study, a definite conclusion cannot be made. Large randomized control trials are required to confirm the efficacy of Prolotherapy in burn Wounds.
References:
- Oh JY, Choi GE, Lee HJ. High-glucose-induced reactive oxygen species stimulates human mesenchymal stem cell migration through snail and EZH2-dependent E-cadherin repression. Cell PhysiolBiochem. 2018; 46:1749–1767.
- Penn JW, Grobbelaar AO, Rolfe KJ. The role of the TGF-β family in wound healing, burns and scarring: a review. Int J Burns Trauma. 2012; 2:18–28
- Freeman JW, Empson YM, Ekwueme EC, Paynter DM, Brolinson PG. Effect of prolotherapy on cellular proliferation and collagen deposition in MC3T3-E1 and patellar tendon fibroblast populations. Transl Res. 2011; 158:132–139.
- Wu TJ, Fong YC, Lin CY, Huang YL, Tang CH. Glucose enhances aggre can expression in chondrocytes via the PK Calpha/p38-miR141–3p signalling pathway. J Cell Physiol. 2018; 233:6878–6887.
- Topol GA, Podesta LA, Reeves KD. Chondrogenic effect of intra-articular hypertonicdextrose (Prolotherapy) in severe knee osteoarthritis. PMR. 2016; 8:1072–1082
